Peyronie’s disease is a complex and often misunderstood condition that affects the structure and function of the penis. It is characterized by the formation of fibrous scar tissue—known as plaques—within the penile shaft, which can lead to abnormal curvature, pain, and sexual dysfunction. Although it is not life-threatening, Peyronie’s disease can significantly impact a man’s confidence, intimate relationships, and overall quality of life.
This detailed guide provides a comprehensive exploration of Peyronie’s disease, including its underlying mechanisms, risk factors, symptoms, stages, diagnostic methods, treatment strategies, and psychological implications.
Understanding the Anatomy: How Peyronie’s Disease Develops
To understand Peyronie’s disease, it is important to first look at the anatomy of the penis.
The penis contains two cylindrical chambers called the corpora cavernosa, which fill with blood during an erection. These chambers are surrounded by a strong, elastic layer known as the tunica albuginea. In a healthy penis, this tissue stretches evenly, allowing a straight erection.
In Peyronie’s disease, fibrous scar tissue forms within the tunica albuginea. Unlike normal tissue, these plaques are rigid and do not stretch. When an erection occurs, the unaffected side expands normally, while the scarred side remains restricted—causing the penis to bend or curve.
Causes and Risk Factors
The exact cause of Peyronie’s disease is not always identifiable, but research suggests a combination of physical trauma and biological predisposition.
1. Repeated Microtrauma
Minor, often unnoticed injuries to the penis during sexual activity are considered the most common trigger. These injuries may cause internal bleeding and inflammation, leading to scar formation.
2. Acute Injury
A sudden, more severe injury—such as bending of the erect penis—can initiate plaque formation.
3. Genetic Predisposition
Men with a family history of Peyronie’s disease or connective tissue disorders are more susceptible. This suggests a genetic tendency toward abnormal wound healing.
4. Age-Related Changes
As men age, tissue elasticity decreases, and healing processes become less efficient, increasing the risk of scar formation.
5. Associated Conditions
Certain health conditions are linked to Peyronie’s disease:
- Diabetes mellitus
- Hypertension
- Erectile dysfunction
- Dupuytren’s contracture (thickening of hand tissues)
6. Lifestyle Factors
- Smoking (affects blood vessels and healing)
- Poor cardiovascular health
- Sedentary lifestyle
Symptoms: Recognizing the Signs Early
Symptoms can vary significantly in severity and progression. Early detection is key to effective management.
1. Penile Curvature
The most defining symptom is a bend in the erect penis. The curvature can:
- Develop gradually or suddenly
- Be mild (barely noticeable) or severe (greater than 30–60 degrees)
- Occur in any direction
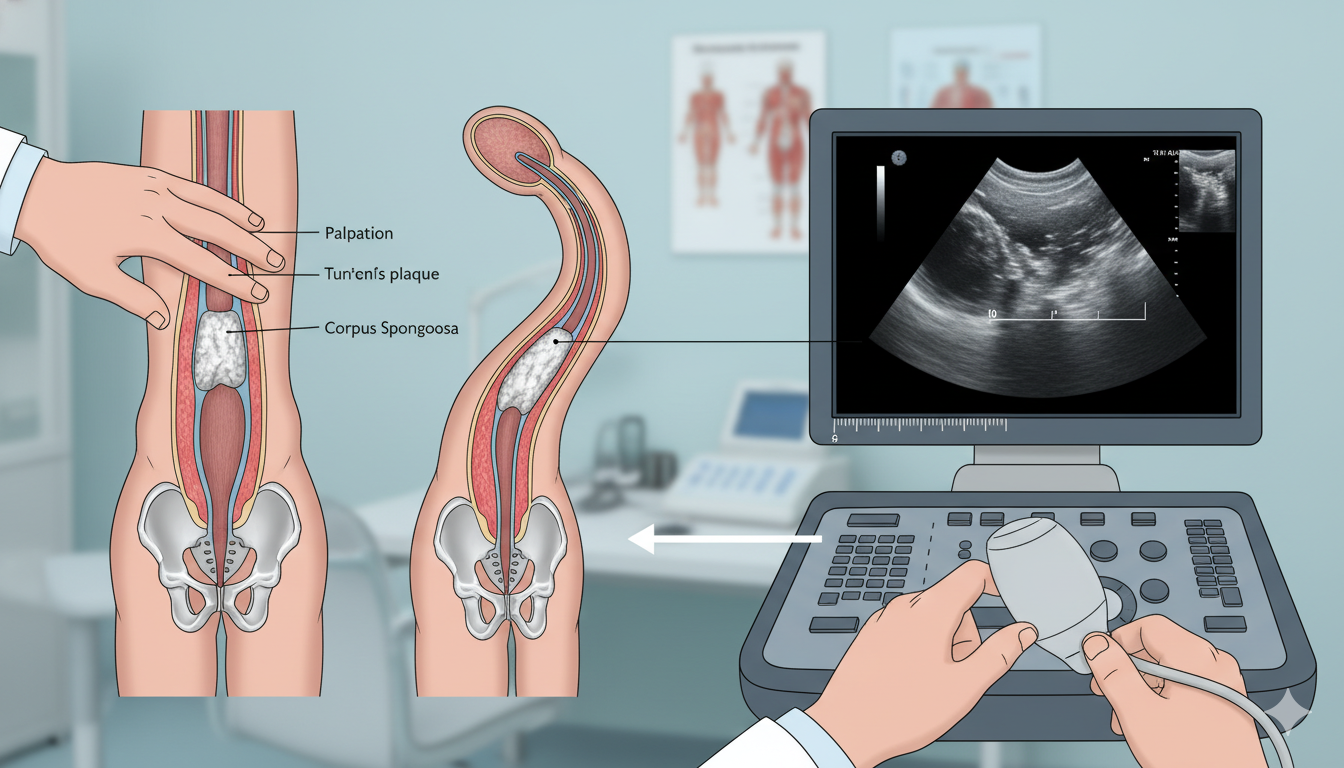
2. Palpable Plaques
Patients may feel hardened areas or lumps under the skin. These plaques can vary in size and may be tender in the early stages.
3. Pain
Pain is more common during the acute phase and may:
- Occur during erection
- Occasionally persist in the flaccid state
- Gradually decrease over time
4. Erectile Dysfunction (ED)
ED may result from:
- Reduced blood flow
- Psychological stress
- Structural changes in the penis
5. Penile Shortening
Scar tissue reduces elasticity, which can lead to noticeable shortening.
6. Complex Deformities
In advanced cases, deformities may include:
- Hourglass narrowing
- Indentations
- Hinging effect (instability during erection)
Disease Progression: Acute vs Chronic Phase
Peyronie’s disease progresses through two distinct stages:
Acute Phase (Active Phase)
- Duration: 6 to 18 months
- Active inflammation and plaque formation
- Increasing curvature
- Pain is most prominent
Chronic Phase (Stable Phase)
- Pain subsides
- Curvature stabilizes
- Plaques become firm and permanent
- Ideal time for surgical intervention if needed
Diagnosis: Clinical and Imaging Evaluation
1. Medical History
Doctors assess:
- Duration of symptoms
- Degree of curvature
- Pain intensity
- Sexual function
2. Physical Examination
The penis is examined for:
- Plaque location and size
- Degree of deformity
3. Ultrasound Imaging
Penile ultrasound is the most useful diagnostic tool. It helps:
- Visualize plaques
- Detect calcification
- Assess blood flow
4. Induced Erection Test
In some cases, medication is used to create an erection in a clinical setting to measure curvature accurately.
Treatment Options: A Comprehensive Overview
Treatment depends on:
- Severity of curvature
- Stage of disease
- Presence of erectile dysfunction
- Patient preference
Non-Surgical Treatments
1. Oral Medications
Though widely used, results vary:
- Vitamin E (antioxidant)
- Potaba (may reduce plaque size)
- Anti-inflammatory drugs
2. Intralesional Injections
These are among the most effective non-surgical treatments.
Collagenase Clostridium Histolyticum (CCH)
- Breaks down collagen in plaques
- Can significantly reduce curvature
- Administered in cycles
Verapamil
- Improves blood flow and reduces scar tissue
Interferon-alpha-2b
- Reduces inflammation and fibrosis
3. Penile Traction Therapy (PTT)
A mechanical device is used to stretch the penis gradually. Benefits include:
- Reduced curvature
- Increased length
- Prevention of further deformity
Patients typically need to use the device for several hours daily over months.
4. Vacuum Erection Devices (VED)
These devices improve blood flow and may:
- Enhance penile health
- Reduce curvature when used consistently
5. Shockwave Therapy
Low-intensity extracorporeal shockwave therapy (Li-ESWT) is used primarily to:
- Reduce pain
- Improve tissue healing
However, its effect on curvature is still under investigation.
Surgical Treatment Options
Surgery is considered when:
- Curvature prevents intercourse
- Disease is stable for at least 6 months
- Non-surgical treatments fail
1. Penile Plication
- Shortens the longer side
- Straightens the penis
- Simpler procedure
- May reduce penile length
2. Plaque Incision/Excision with Grafting
- Plaque is cut or removed
- Graft is placed to restore shape
- Suitable for severe curvature
- Higher risk of erectile dysfunction
3. Penile Prosthesis (Implant)
Recommended for men with severe ED:
- Inflatable or semi-rigid implants
- Correct curvature and restore function
- High satisfaction rates
Psychological and Relationship Impact
Peyronie’s disease affects more than physical health—it can deeply impact emotional well-being.
Common Psychological Effects:
- Anxiety and depression
- Reduced self-confidence
- Fear of intimacy
- Relationship strain
Coping Strategies:
- Open communication with partner
- Counseling or sex therapy
- Support groups
Mental health support is often as important as medical treatment.
Lifestyle Modifications and Self-Care
Although lifestyle changes cannot cure Peyronie’s disease, they can improve overall outcomes.
Healthy Habits:
- Quit smoking
- Maintain a balanced diet
- Exercise regularly
- Manage stress
Sexual Health Tips:
- Use lubrication
- Avoid aggressive movements
- Choose comfortable positions
Medical Management:
- Control diabetes and blood pressure
- Monitor erectile function
Complications of Untreated Peyronie’s Disease
If left untreated, the condition may lead to:
- Severe curvature
- Permanent deformity
- Chronic erectile dysfunction
- Emotional distress
Prognosis and Recovery
The outlook varies:
- Some men stabilize without treatment
- Others require medical or surgical intervention
- Early treatment improves success rates
Modern therapies offer effective solutions, and many men regain satisfactory sexual function.
Prevention: Is It Possible?
While complete prevention is not guaranteed, risk can be reduced by:
- Avoiding penile trauma
- Practicing safe sexual techniques
- Managing chronic diseases
- Seeking early medical advice
Frequently Asked Questions (FAQs)
Is Peyronie’s disease permanent?
Not always. Some cases stabilize or improve, but others may require treatment.
Can it go away on its own?
Mild cases may improve, but significant curvature usually persists without treatment.
Is it related to cancer?
No, Peyronie’s disease is not cancerous.
Does it affect fertility?
It does not directly affect fertility but may interfere with sexual activity.
Final Thoughts
Peyronie’s disease is a multifaceted condition that requires a comprehensive approach to diagnosis and treatment. While it can be physically and emotionally challenging, advancements in medical science have made it increasingly manageable.
Early intervention, personalized treatment plans, and psychological support are key to achieving the best outcomes. If you or someone you know is experiencing symptoms, seeking professional medical advice is the most important step toward recovery and improved quality of life.
More Recommended
